Surprise: HDAC Goes Down, Not Up, in Alzheimer’s Disease
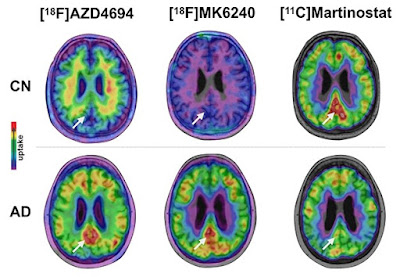
As gene regulation changes in Alzheimer’s disease, scientists believe that histone deacetylases (HDACs) go into overdrive, shutting down transcription of certain genes. Consequently, several research groups are exploring the potential of HDAC inhibitors as AD therapeutics, with at least two trials currently enrolling. The recent development of a PET tracer that recognizes class I HDACs in the brains of living people provides a valuable tool for such trials. Now, however, the first HDAC PET data from people with AD upends previous findings. Tharick Pascoal of McGill University, Montreal, reported that HDAC levels drop as disease advances. “That was a surprise to us. We expected the opposite result,” Pascoal told Alzforum. At first, the researchers worried that there might be errors in their methodology; however, validation by a second group studying an independent cohort convinced them the finding was real, and robust. “I’ve never seen two independent PET studies where th...





















